SANTA CLARA, Calif.,
|
|||||||||||||
iMIA is a Level 1 RCT, conducted at nine hospitals in four countries in Europe, that assessed the safety and effectiveness of SI joint fusion (SIJF), also referred to as SI joint arthrodesis in the manuscript, with the triangular iFuse Implants compared to conservative management (CM) in patients with chronic SI joint dysfunction. The JBJS publication, titled Randomized Trial of Sacroiliac Joint Arthrodesis Compared with Conservative Management for Chronic Low Back Pain Attributed to the Sacroiliac Joint,1 showed that minimally invasive SIJF with iFuse Implants was safe and more effective than CM in relieving pain, reducing disability, and improving patient function and quality of life at two years.
“What I find remarkable is the consistency of the results between the 2-year iMIA and 2-year INSITE RCTs,” said David Polly, Jr., MD, Professor,
The iMIA 2-year results were published in JBJS, which has an impact factor of 4.84, the highest among orthopedic journals, and is a highly valued source of information for orthopedic surgeons and researchers. As such, this publication, which is the 67th peer-reviewed iFuse publication, is a significant indication of the broad acceptance of SI joint surgery as an important topic of study in orthopedics.
“The publication of this Level 1 study in a prestigious orthopedic journal such as JBJS is an important milestone signaling recognition of the sacroiliac joint, like all other joints in the human body, as a pain generator and acknowledgement of the high quality of evidence that supports iFuse as an effective minimally invasive procedure for patients with SI joint pain”, said Daniel Cher, MD, Vice President of Clinical Affairs at
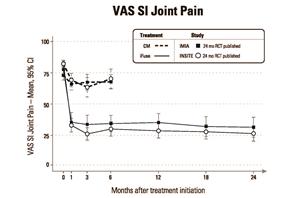
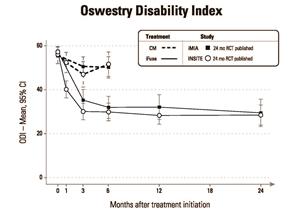
As shown in Figures 1 and 2 below, 2-year results from iMIA were remarkably consistent with 2-year results from INSITE (Investigation of Sacroiliac Fusion Treatment – NCT01681004), the RCT conducted at 19 institutions in the U.S. and published in August, 2016 in the
In the iMIA study, 103 subjects were randomly assigned to CM (n=51) or SIJF (n=52) between
About SI-BONE
SI-BONE is a medical device company that pioneered the iFuse Implant System, a minimally invasive surgical system for fusion of the sacroiliac joint to treat sacroiliac joint dysfunction. The SI joint is the last major joint with a clinically proven surgical treatment. The iFuse Implant, commercially available since 2009, is the only SI joint fusion device supported by multiple prospective clinical studies showing improved pain, patient function and quality of life resulting from treatment. There are more than 65 peer-reviewed publications supporting the safety, durable effectiveness, and biomechanical and economic benefits unique to the iFuse Implant (www.si-bone.com/results). This body of evidence has enabled multiple government and private insurance payors to establish coverage of the SI joint fusion procedure exclusively when performed with the iFuse Implant System.
The iFuse Implant System is intended for sacroiliac fusion for conditions including sacroiliac joint dysfunction that is a direct result of sacroiliac joint disruption and degenerative sacroiliitis. This includes conditions whose symptoms began during pregnancy or in the peripartum period and have persisted postpartum for more than 6 months. There are potential risks associated with the iFuse Implant System. It may not be appropriate for all patients and all patients may not benefit.
SI-BONE and iFuse Implant System are registered trademarks of
- Dengler J, Kools D, Pflugmacher R, Gasbarrini A, Prestamburgo D, Gaetani P, Cher D, Van Eeckhoven E, Annertz M, Sturesson B. Randomized Trial of Sacroiliac Joint Arthrodesis Compared with Conservative Management for Chronic Low Back Pain Attributed to the Sacroiliac Joint. J Bone Joint Surg. 2019;101(5):400-411. doi: 10.2106/JBJS.18.00022
- Polly DW, Swofford J, Whang PG, Frank CJ, Glaser JA, Limoni RP, Cher DJ, Wine KD, Sembrano JN, and the
INSITE Study Group . Two-Year Outcomes from a Randomized Controlled Trial of Minimally Invasive Sacroiliac Joint Fusion vs. Non-Surgical Management for Sacroiliac Joint Dysfunction. Int J Spine Surg. 2016;10:Article 28. doi: 10.14444/3028
Contact:
For
Joe Powers
Vice President of Marketing
669-206-2521
jpowers@si-bone.com
Photos accompanying this announcement are available at
http://www.globenewswire.com/NewsRoom/AttachmentNg/6d116c9c-0bf2-452c-a154-672ac3b2df8f
http://www.globenewswire.com/NewsRoom/AttachmentNg/742f9332-30ef-4f2a-a04f-7eae432dbe0b
Source: SI-BONE, Inc.